Original Article Medical
Physics
Experience with the use of a dose management system in the
everyday routine of a CT department. A touchstone or a millstone?
Virginia Tsapaki1, Niki Fitousi2, Alexandros Salametis3, Dimitrios Niotis4, Ioannis Papailiou5
1 Medical Physicist,
Konstantopoulio Hospital, Nea Ionia, Athens, Greece
2 Medical Physicist,
Qaelum NV, Gaston Geenslaan 9, B-3001 Leuven, Belgium
3 Medical Physicist,
Konstantopoulio Hospital, Nea Ionia, Athens, Greece
4 Radiographer,
Konstantopoulio Hospital, Nea Ionia, Athens, Greece
5 Radiologist,
Konstantopoulio Hospital, Nea Ionia, Athens, Greece
Submission: 13/7/2017 |
Acceptance: 5/2/2018
Abstract
Purpose: A dose
tracking software was recently installed in our CT department. The study aimed
at evaluating the software capabilities and staff performance in every day
routine.
Material and Methods: A dose
tracking software was connected to a 64-slice CT scanner. All technical and
dosimetric data of 6,010 CT examinations were analysed. Organ doses estimated
by the software were also evaluated.
Results: The software
provided easy and quick statistical overview of clinical and technical data.
Typical local doses were comparable to national and international data. Organ
doses proved to be an instrumental and supportive tool in individualised
patient dosimetry.
Conclusions: The
software offered easy and quick statistical overview of all CT clinical and
technical data and a valuable overview of workload statistics, which occasionally
required discussion with the staff and, in some cases, corrective actions. It
easily provided the time periods the scanner was not in use, and facilitated
easy scheduling of routine quality control tests and other routine tasks in the
department. A number of errors were identified and communicated to the staff;
corrective actions were taken.
Key words
CT; Dose; Tracking software; Optimisation;
Management
Corresponding Author,
Guarantor
Virginia
Tsapaki
Konstantopoulio
Hospital, 3-5 Agias Olgas Str, Nea Ionia 142 33, Athens, Greece
E-mail: virginia@otenet.gr
1. Introduction
CT is widely used in diagnosis of disease and
has been identified as the major contributor to the collective radiation dose
to population from medical exposures [1-7]. Depending on clinical needs and
technical protocols, patient radiation dose differs, even for the same
anatomical region, clinical indication, technical protocol and sometimes even
for the same CT unit [8-12]. Furthermore, high rates of repeated CT scans are
reported in the literature (such as in trauma patients) with additional hospital
charges and additional radiation exposure [13]. The urge to monitor medical
practices in CT scanner has risen significantly. The effective dose (E) for
the most typical CT examinations varies tremendously even for the same
technical protocol or the same CT scanner (1 mSv- 25 mSv) [8-23]. Therefore,
the necessity of tracking patient dose data and CT scanning protocols is
essential. It is worth noticing that CT radiation dose is linked to an increased
risk of radiation-induced cancer [24-26].
To assess the radiation dose
in CT, volumetric computed tomography dose index (CTDIvol), dose length
product (DLP) and E are the most widely used radiation dose indices [8, 10,
27]. In order to optimise radiological practices more efficiently in terms of
radiation dose, the term Diagnostic Reference Level (DRL) is defined both in
the European [28] and International [29] Basic Safety Standards (BSS). It is
also clearly stated that medical X-ray equipment must have a means to inform
the practitioner of the relevant parameters for assessing the patient dose and,
even more important, to have the capacity to transfer this information to the
record of the examination [29].
Due to the upcoming
implementation of the EU BSS [29], the need for an automated dose monitoring
solution rises. This can be an extremely time consuming and complex task.
Nowadays, sophisticated software packages with friendly interface can assist
to this task, resulting in a much easier and quicker way to monitor all data
included in the Digital Imaging and Communication in Medicine (DICOM) header of
the CT scanner or data recorded in the Picture Archiving and Communication System
(PACS) of the hospital [30-37]. These studies focus on radiation dose data
analysis.
One of the commercially
available dose tracking software was recently installed in our CT department.
Our study focused on evaluating the software features and capabilities and on
assessing staff performance in every day routine. It also investigated whether
the system can be used solely for patient radiation dose analysis, or could
also assist in the general management of the CT department.
2. Material and Methods
2.1 CT scanner and dose tracking software system
A dose tracking software (DOSE, Qaelum,
Belgium) was recently connected to a Philips Brilliance 64 CT scanner (Philips
Systems, the Netherlands), installed in 2013 in Konstantopoulio General
Hospital in Athens, Greece. This is a software tool that has the capability to
connect with a variety of medical ionising and non-ionising radiation units
that are available in a hospital and to combine all available data into a
single configuration where every examination is analysed and archived. The configuration
provides a direct overview and makes information available at any time for all
users, depending on their level of authority. Although initially intended to be
connected to a number of X-ray modalities such as an angiography system, an
older four (4) slice CT scanner and certain computed radiography systems, this
could not be done in real practice. This was due to the fact that these devices
are old and they could not export dose data in the DICOM formats that the
software supports. It must be noted that our hospital does not have a PACS
system and therefore the software was connected directly to the Philips
64-slcie CT scanner.
2.2 Technical factors and dosimetric quantities collected
For each examination, the tube voltage (kV), tube output
(mAs), Field of View (FOV), pitch, collimation, number of slices, series
information, scanogram and operator’s name are examples of clinical data that
can be recorded. Regarding radiation dose metrics, CTDIvol and DLP are the
dosimetric quantities transferred from the CT scanner to the software
workstation. The software uses the patient CT exam data and calculates E and
organ doses. Organ doses are estimated using conversion factors derived from
Monte Carlo simulations for a standard-size model. More specifically, the
conversion factors are derived by an in-house Monte Carlo simulation model
that has been developed based on vGate simulation tool. A reference adult
phantom from the phantom library of MIRD is used for the simulations. The
model calculates the organ doses for every body part examined according to
typical z-ranges. Specifically, for every organ, dose profiles are generated.
Simulated scans are performed per 1 cm in the z-direction for various photon energies
up to 140 keV obtained by combining different energy values according to the
realistic spectrum for a given tube voltage. For organs away from the scan
range, extrapolation of sparse data is performed. Organ doses are derived by
adding the values of the dose profile over the typical z-range (determined by
typical examination types). The validation of the in-house model was already
performed against commercially available dosimetric tools before the study to
ensure accuracy of organ dose estimation [38].
2.3
Patient sample
The
study included 6,010 CT examinations from 13th March 2016 to 14th March 2017.
The study was performed according to the ethical standards as described by the
Declaration of Helsinki. Initially an overall evaluation of all CT
examinations and utility of the software was performed. Then a more focused
analysis was performed for the most frequent CT exams independently of
clinical indication. Due to the higher radiosensitivity of organs in
examinations of the trunk, the authors decided to
focus on these exams for further analysis. In order to estimate organ doses,
the examinations were divided in 3 broad anatomical part categories: Chest,
Abdomen and Chest/Abdomen/Pelvis (CAP) CT examinations.
3. Results
3.1 Overall evaluation
The percentage of men and women were 41% and
59%, respectively. The software offered easy and quick statistical overview of
all clinical and technical data of CT examinations. This overview could be
provided for a specific date, for a time period within the day, or for a whole
date range selected by the user. An example of this workload overview can be
seen in Fig. 1a and 1b. Fig. 1a shows the evaluation of each hour
and day of the week in the CT room, in terms of number of performed examinations
and average DLP. The number of examinations is shown by the size of the boxes;
the mean accumulated DLP is colour coded. It is practically a moment evaluation
chart of the actual usage of the CT scanner plotted together with the
corresponding DLP on a certain day and hour. Thus, the volume and dose trends
are visualised to facilitate the analysis. The more red the box becomes, the
more radiation dose (in terms of DLP) is given to the patients the specified
time of the day. As the box becomes bigger in size, the higher is the number of
exams. This provided a valuable overview of the workload statistics which
occasionally required discussion with the related staff and in some cases,
corrective actions. Fig. 1b shows a weekly workload analysis graph, that
practically monitors the activity in blue and green colours and also the
inactivity of the CT scanner (orange and red colour). Regular evaluation of
this graph helped optimise the use efficiency of the scanner. It also allowed
making changes in the number of technologists in every day routine for better
management of the department. This also identified in a more structured way
the time periods the scanner was not in use, in order to schedule routine
quality control tests.
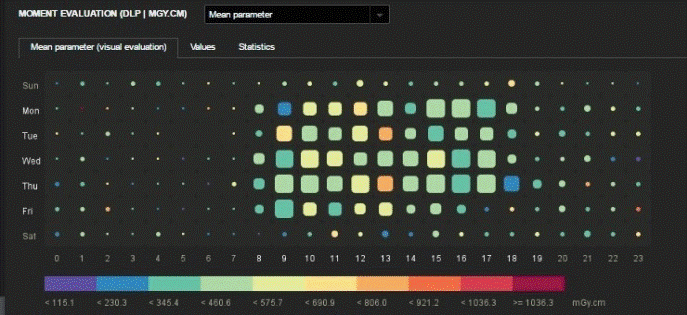
Fig. 1a. The
graph shows an evaluation of the number of examinations performed in the CT
room and the average DLP as a function of hours and days in the week. The
number of exams represents the size of the boxes; the mean accumulated dose
length product (DLP) is colour coded
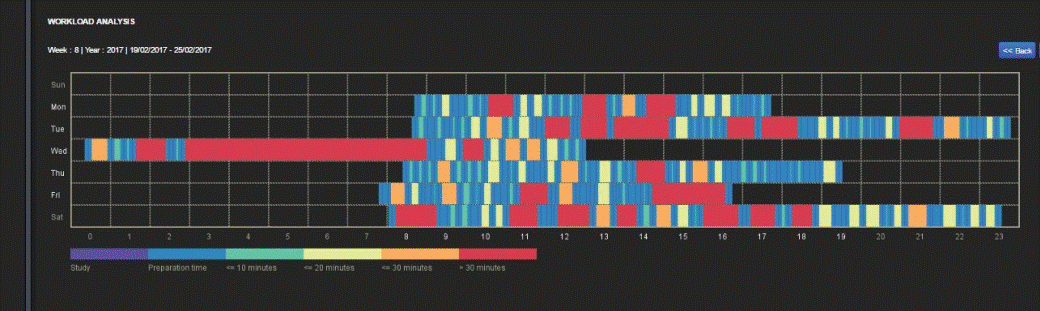
Fig. 1b. The graph shows the analysis of the
weekly workload of the CT scanner as a function of hours and days in the week.
The bar below the graph defines the colours related to the time periods of the
usage. Starting from purple on the left ending to red on the right, the colour
bars show: 1) the actual study, 2) the preparation time, 3) time gap of less
than 10 min, 4) time gap of less than 20 min, 5) time gap of less than 30 min
and finally 6) time gap of more than 30 min.
The software allowed evaluation of patient demographics,
in multiple ways depending on the operator or hospital management needs. Fig.
2 shows part of patient demographics analysis. It presents the
distribution of patient sample according to age, separately for men and women.
It shows that most of patients are in the range of 60-90 years, whereas the
percentage of patients in the 40-60 years range is much smaller. This could be
partially explained by the fact that European population is aging and a rise of
chronic diseases is recorded [39].
As far as technical protocols and parameters used are concerned, a
very large variability of CT protocols was noticed. Forty six (46) different
scanning protocols were recorded for 16 different anatomical regions. These protocols
are related both to anatomical region and clinical indication. It must be noted
that effective dose and organ doses estimation are related to anatomical
region and not clinical indication. The analysis revealed mistakes in the
technique mainly related to the technical protocol (extra image series, longer
scans than actually needed, wrong protocolused, or even choosing the correct
protocol but typing the wrong name). All these errors were communicated to the
operators and helped in the optimisation of procedures and better organisation
of the department.
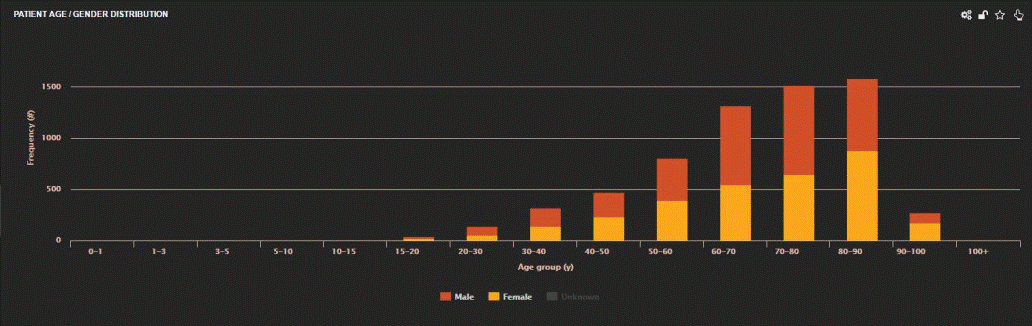
3.
Fig. 2. Distribution (%) of patient sample according to age is presented.
The yellow bar represents the female patients and the orange bar the male
patients.
2 Dose evaluation
Table 1 shows median value
and range for CTDIvol, DLP and E for routine chest and abdomen, as well as CAP
examinations. Minimum dose values were found for Chest CT, followed by
Abdomen CT and CAP exam. CTDIvol values did not have big differences between
exam protocols. On the other hand, DLP almost doubled from Chest to Abdomen and
more than tripled from Chest to CAP exam. For E, the value increased about 1.6
times from Chest to Abdomen and 2 times from Chest to CAP exam. The large range
in DLP andE values especially in CAP reflected the protocol variability. This
could be partially explained by different number of series (pre-contrast,
post-contrast studies, multiphase studies, etc.) depending on clinical
indication and physician choice. Another reason was the different scan range
applied by some operators. This was further investigated and results are
presented in the last paragraph of this section. In general, all findings were
discussed with radiologists and technologists and corrective actions were
taken.
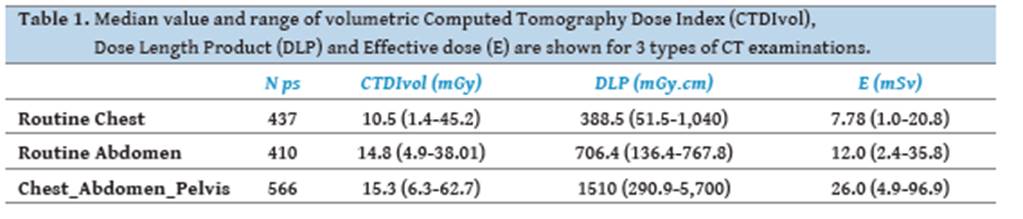
Table 2 defines
typical local DRLs in terms of CTDIvol (mGy) and DLP (mGy.cm). They are defined
based on the methodology described in the European CommissionGuidance document
on DRLs for medical exposures [40].
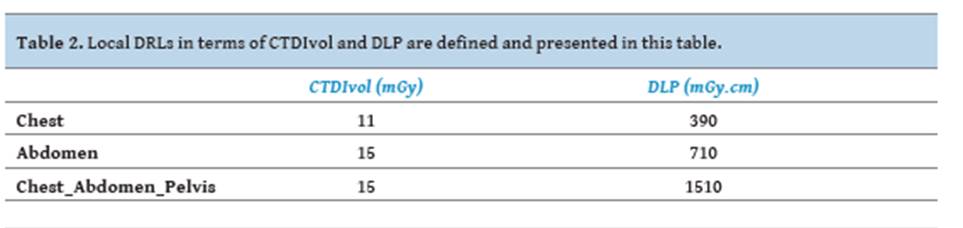
Table
3 presents the comparison of typical local DRLs to national and
international data found in the recent literature. It is noted that in almost
all cases our local values are lower than both national and international data.
The only local DRL higher than international data was for the CAP exam. As
CTDIvol was comparable with the literature data, it is obvious that the
scanning length was the reason for the higher CAP DLP.
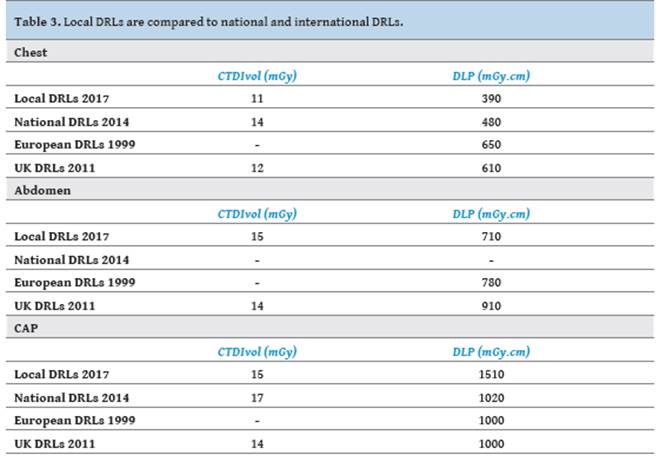
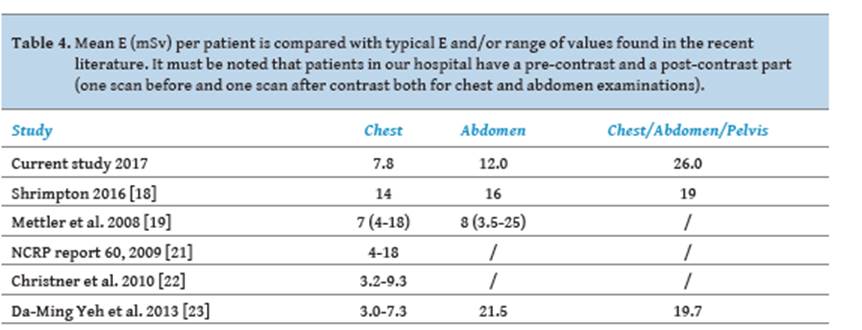
Table 4 presents the
comparison of E with international literature [18, 19, 21-23]. It must be noted
that our data are based on the fact that our routine examinations are performed
with a pre-contrast and a post-contrast scan. Some of the papers listed in the
table [23] specify values both per scan and per patient. Others do not clarify
if values reported are for one or two scans (pre contrast or both pre and post
contrast scans). It is evident that this plays a very important role for the
final value of E. The large variability of doses reflects the large
differences in technical protocols that most often depend on clinical
indication, or the differences in scan length (usually the choice of operator).
The software also offers individual organ doses (mGy) estimation
in routine basis. Apart from individual patient organ doses, the software
calculates the 25 percentile, median values and 75 percentile for the organ
doses. There is also the possibility to calculate these values for the whole
sample of patients or apply a filter based on the specific body part or the
same description of the examination. An example is given in Fig. 3a and 3b.
In Fig. 3a, organ doses are shown for a male patient undergoing a multi
phase CAP examination receiving an E of 96.9 mSv. The figure shows the organ
doses in orange bars compared to the 25% of the whole patient sample
distribution (yellow bars), the median (blue bars) and 75% (green bars). In Fig.
3b, organ doses are shown in a similar way for a male patient undergoing a
single phase CAP examination receiving a low E dose of 6.5 mSv. The bar graphs
of the 2 figures clearly show that organ doses in a high dose exam can reach
values over 300 mGy in more than one organ (breast, lung, etc.) whereas there
are CT examinations in which no organ receives a dose above 10 mGy (Fig. 3a).
This tool was used in specific patient to patient dose evaluation and as an
educational means for optimisation purposes. In certain cases, it was helpful
to estimate quickly organ doses in women of reproductive age in case of anxiety
following a CT exam (this reassured the patient that radiation dose was
minimal).
DLP is the dose value that represents more efficiently the
differences between radiographers due to the differences in scan length (Fig.
4). Chest CT is a straightforward standard examination, which is performed
in a similar way in terms of DLP by all radiographers. Abdomen and even more
the CAP examinations vary in terms of DLP, due to the different scan region.
This was also communicated and further discussed with radiographers and
radiologists. As the software has a simulation tool that estimates organ and
effective dose for different technical CT factors, it was used for educational
purposes to show in a more efficient way the effect of scan length (as well as
all technical CT factors) in radiation dose.
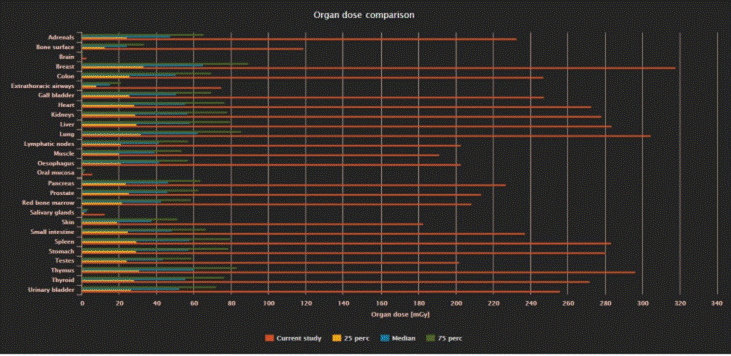
Fig.3a. Organ doses in mGy are shown for a)
a patient with high dose values (orange bars) compared to 25% (yellow bars),
median (blue bars) and 75% (green bars) organ doses of the whole patient sample
and for b) a patient with low dose values. a) Male patient, CAP
examination, E: 96.9 mSv, b) Male patient, CAP examination, E: 6.5 mSv.
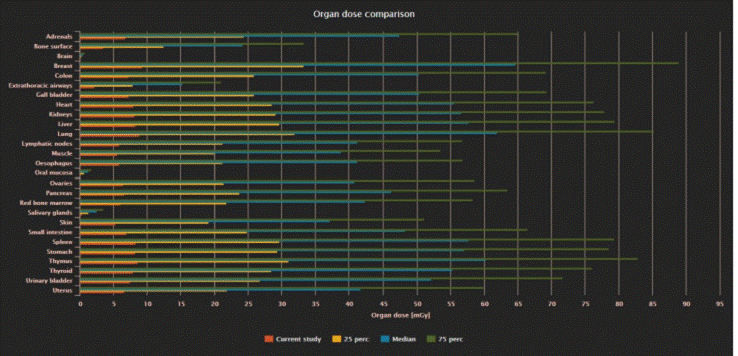
Fig.3b. Male patient, CAP
examination, E: 6.5 mSv.
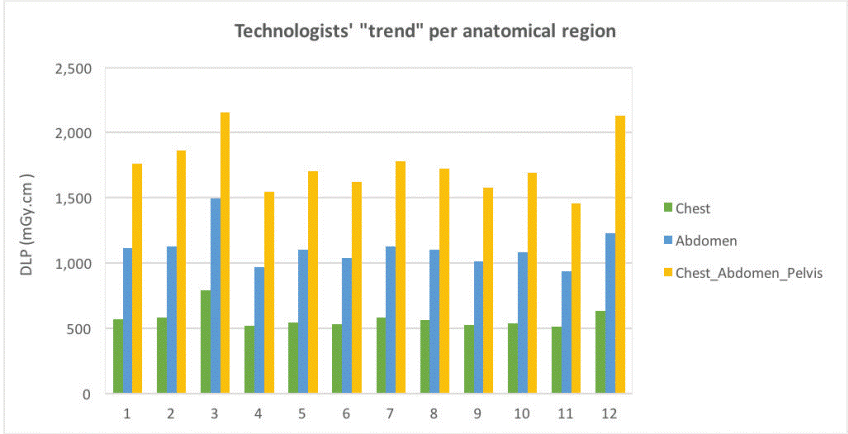
Fig. 4. Radiographer “habits”
in relation to DLP are shown.
4. Discussion
The dose management system proved to be an effective, powerful
tool that facilitated the evaluation of general practice and workflow of the
CT department and revealed the habits of operators, so that corrective actions
are made for the benefit of the patient. Before installing the software,
analysis of data was a cumbersome process that required manual entry of
values, with significant outflow of resources and the risk of typing errors.
The fact that all these had to be done manually patient by patient was the main
reason why it could not be done in a systematic way.
One could argue that the
implementation of a dose management system is a cost for the hospital,
especially with the current financial situation in Greece. This cost, which
usually increases with the number of X-ray devices or examinations performed,
includes not only the installation but also the maintenance. However, the gain
of the hospital is also important. In this study, we highlighted some parts of
the benefit, mostly in terms of improvement of workload, personnel efficiency
and patient dose evaluation. As far as radiation doses are concerned,
assessment of examination doses in terms of CTDIvol and DLP for a certain
number of patients is presented and discussed extensively in the international
literature for at least 20 years. The use of the dose tracking tool to evaluate
the whole sample and not only a limited number of patients helped to easily
identify weaknesses and mistakes in our every day routine. The immediate
estimation of E and organ doses proved to be a valuable tool in this process.
It allowed us to take a deep dive into the patient data for optimisation of
safety, quality, training and practice of the department.
The traditional estimation of average CTDIvol,
DLP and E and comparison with national or international values seems no longer
relevant, if one considers the numerous and very different technical protocols
applied for different clinical indications for the same anatomical region.
Furthermore, the number of scanning phases depends also on the clinical
indication which is basically the main determining factor of radiation dose.
Various clinical indication–specific CT technical protocols have been developed
to help tailor CT dose and image quality on the basis of specific clinical
indications. It seems essential to define diagnostic reference levels for each
of these clinical indications for more accurate comparison of practice. R
Conflict of interest
The authors declared no
conflicts of interest.
References
1. Mori S, Endo M, Nishizawa K, et al. Comparison of patient doses
in 256-slice CT and 16-slice CT scanners. Br J Radiol
2006; 79: 56–61.
2. Silverman JD, Paul NS, Siewerdsen JH. Investigation of lung nodule
detectability in low-dose 320-slice computed tomography. Med Phys 2009; 36(5): 1700-1710.
3. Kalra MK, Woisetschläger M, Dahlström N, et al. Sinogram-affirmed
iterative reconstruction of low-dose chest CT: Effect on image quality and
radiation dose. AJR Am J Roentgenol 2013; W235-W244.
4. Gaztanaga J, Garcia MJ. New noninvasive imaging technologies in
coronary artery disease. Curr Cardiol Rep 2009; 11(4): 252-257.
5. Pauls S, Gabelmann A, Heinz W, et al. Liver perfusion with dynamic
multidetector-row computed tomography as an objective method to evaluate the
efficacy of chemotherapy in patients with colorectal cancer. Clin Imaging 2009; 33(4): 289-294.
6. Türkvatan A, Olçer T, Cumhur T. Multidetector CT urography of
renal fusion anomalies. Diagn Interv Radiol 2009; 15(2): 127-134.
7. Flor N, Zuin M, Brovelli F, et al. Regenerative nodules in
patients with chronic Budd-Chiari syndrome: A longitudinal study using multiphase
contrast-enhanced multidetector CT. Eur J Radiol 2010; 73(3): 588-593.
8. International Commission on Radiological Protection (ICRP).
Managing patient dose in multi-detector computed tomography (MDCT). Annals of the ICRP 102, 2007. V 37/1,
Elsevier.
9. Shrimpton PC. Protection of the patient in X-ray computed
tomography. Documents of the National Radiological Protection Board (NRPB) 1992;
V 3, N 4 Chilton: NRPB.
10.
Baert AL, Knauth M, Sartor K.
Radiation dose from adult and pediatric multidetector computed tomography. Springer, 2007.
11.
Tsalafoutas IA, Tsapaki V,
Triantopoulou C, et al. CT guided interventional procedures: Patient effective
and skin dose considerations. AJR Am J
Roentgenol 2007; 188: 1479–1484.
12.
Mayo-Smith WW, Hara A, Mahesh M, et
al. How I do it: Managing radiation dose in CT. Radiology 2014; 273(3): 657-672.
13.
Jones AC, Woldemikael D, Fisher T,
et al. Repeated computed tomographic scans in transferred trauma patients:
Indications, costs, and radiation exposure. J Trauma
Acute Care Surg 2012; 73(6): 1564-1569.
14.
United Nations Scientific Committee
on the Effects of Atomic Radiation (UNSCEAR) 2008. Report to the General
Assembly, V I: (Sources) Report to the General Assembly, Scientific Annex A,
United Nations, New York, 2010.
15.
Griffey RT, Sodickson A. Cumulative
radiation exposure and cancer risk estimates in emergency department patients
undergoing repeat or multiple CT. AJR Am J
Roentgenol 2009; 192(4): 887-892.
16.
Tsapaki V, Rehani M. Dose
management in CT facility. Biomed Imaging Interv J 2007; 3(2):e43.
17.
Report of American Association of
Physicists in Medicine (AAPM) Task Group 23. CT Dosimetry: The measurement,
reporting, and management of radiation dose in CT. AAPM Report 96, One Physics Ellipse, College Park, 2008.
18.
Shrimpton PC, Jansen JT, Harrison
JD. Updated estimates of typical effective doses for common CT examinations
in the UK following the 2011 national review. Br J Radiol 2016; 89: 20150346.
19.
Mettler FA, Huda W, Yoshizumi TT,
et al. Effective doses in radiology and diagnostic nuclear medicine: A catalog.
Radiology 2008; 248: 254–263.
20.
McCollough CH, Bushberg JT,
Fletcher JG, et al. Answers to common questions about the use and safety of
CT scans. Mayo Clin Proc 2015; 90(10): 1380-1392.
21.
National council on radiation
protection and measurements (NCRP). NCRP Report No. 160 - Ionizing radiation
exposure of the population of the United States, Bethesda, MD, USA, 2009.
22.
Christner JA, Kofler JM, McCollough
CH. Estimating effective dose for CT using dose-length product compared with
usingorgan doses: Consequences of adopting international commission on
radiological protection publication 103 or dual-energy scanning. AJR Am J Roentgenol 2010; 194:
881-889.
23.
Yeh DM, Tsai HY, Tyan YS, et al.
The Population effective dose of medical computed tomography examinations in
Taiwan for 2013. Jagetia GC 2016, ed. PLoS ONE. 11(10): e0165526. doi:10.1371/journal.
pone.0165526.
24.
Brenner DJ, Doll R, Goodhead DT, et
al. Cancer risks attributable to low doses of ionizing radiation: Assessing
what we really know. Proc Natl Acad Sci USA 2003; 100: 13761-13766.
25.
Brenner DJ, Hall EJ. Computed
tomography-an increasing source of radiation exposure. N Engl J Med 2007; 357: 2277-2284.
26.
Brenner DJ. Should we be concerned
about the rapid increase in CT usage? Rev Environ Health
2010; 25(1): 63-68.
27.
The 2007 recommendations of the
international commission on radiological protection. ICRP publication 103. Ann
ICRP 2007; 37(2-4): 1-332.
28.
European Council Directive
2013/59/Euratom on basic safety standards for protection against the dangers
arising from exposure to ionising radiation and repealing Directives
89/618/Euratom, 90/641/Euratom, 96/29/Euratom, 97/43/Euratom and
2003/122/Euratom. OJ of the EU. L13; 57: 1-73 (2014).
29.
Radiation protection and safety of
radiation sources. International basic safety standards general safety
requirements international atomic energy agency (IAEA) safety standards series
No. GSR Part 3, Vienna, 2014.
30.
Seuri R, Rehani MM, Kortesniemi M.
How tracking radiologic procedures and dose helps: Experience from Finland. AJR
Am J Roentgenol 2013; 200: 771-775.
31.
Duong PA, Little BP. Dose tracking
and dose auditing in a comprehensive computed tomography dose-reduction
program. Semin Ultrasound CT MRI 2004; 35: 322-330.
32.
Nicol RM, Wayte SC, Bridges AJ, et
al. Experiences of using a commercial dose management system (GE DoseWatch) for
CT examinations. Br J Radiol 2015; 5: 20150617.
33.
Hadid L, Waryn MJ, Brillet PY, et
al. Impact of a dose-tracking software and iterative reconstruction technique
on the optimisation of CT protocols. Application to the radiology department of
the hospital group “Avicenne, Jean-Verdier, René Muret”. Physica Medica 2013; 29: e15.
34.
De Bondt T, Mulkens T, Zanca F, et
al. Benchmarking pediatric cranial CT protocols using a dose tracking
software system: A multicenter study. Eur Radiol 2017; 27 (2): 841-850.
35.
Wang J, Molvin L, Marsh D, et al. A
management tool for CT dose monitoring, analysis, and protocol review. Med Phys 2014; 41: 558.
36.
MacGregor K, Li I, Dowdell T, et
al. Identifying institutional diagnostic reference levels for CT with radiation
dose Index Monitoring Software. Radiology 2015; 276 (2): 507-517.
37.
Chatzoglou V, Kottou S,
Nikolopoulos D, et al. Management and optimisation of the dose in computed
tomography via dose tracking software. OMICS J Radiol 2016;
5: 227. doi:10.4172/2167-7964.1000227.
38.
https://qaelum.com/solutions/dose.
Last assessed 27 November 2017.
39.
European semester thematic fiche.
Health and health systems. http//www. Ec.europa.eu/europe2020/
pdf/themes/2016/health_systems_201605.pdf (last assessesed 14 March 2017).
40.
European Commission. Radiation
protection 109. Guidance on diagnostic reference levels (DRLs) for medical
exposures. Directorate-General, Environment, Nuclear Safety and Civil
Protection, 1999.
Ready
- Made Citation
Tsapaki
V, Fitousi N, Salametis A, Niotis D, Papailiou I. Experience with the use of a
dose management system in the everyday routine of a CT department. A touchstone
or a millstone? Hell J Radiol 2018; 3(1): 17-26.









