Clinical Case - Test Yourself Musculoskeletal Imaging
Winging scapula in a young athletic male
Foteini Terezaki, Eirini D. Savva, Rafaela M. Smarlamaki
Department of Radiology, University of Crete, Department of Medical Imaging, University Hospital, Heraklion, Greece
Submission: 1/4/2017 | Acceptance: 17/9/2017
PART A
A 17-year-old male patient, elite track athlete, presented with a winging scapula (Fig. 1). His past medical history revealed a right arm pain lasting for a period of two weeks, two months before presentation. Clinical findings included slight impairment of biceps and right brachioradialis reflexes, as well as right serratus muscle weakness. An electromyography study (EMG) was performed. Axial STIR (Fig. 2), axial T1W (Fig. 3) and coronal STIR (Fig. 4) magnetic resonance (MR) images are shown.
Corresponding Author, Guarantor
Foteini Terezaki
Department of Radiology, University of Crete, Department of Medical Imaging, University Hospital, 71110, Heraklion, Crete, Greece
Email: 94foteini@gmail.com
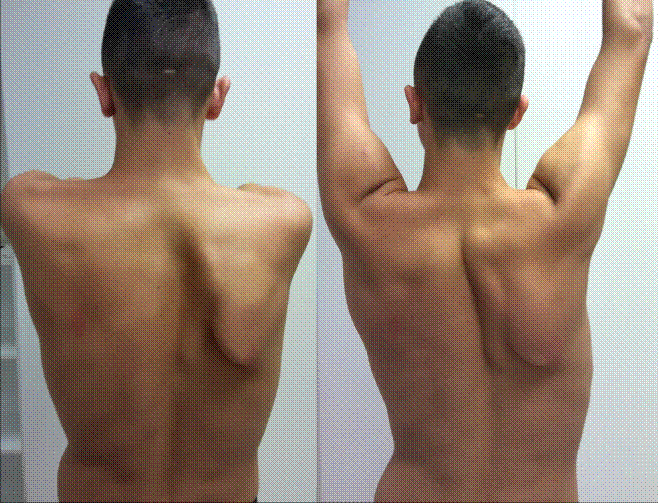
Fig. 1: The patient at clinical examination.
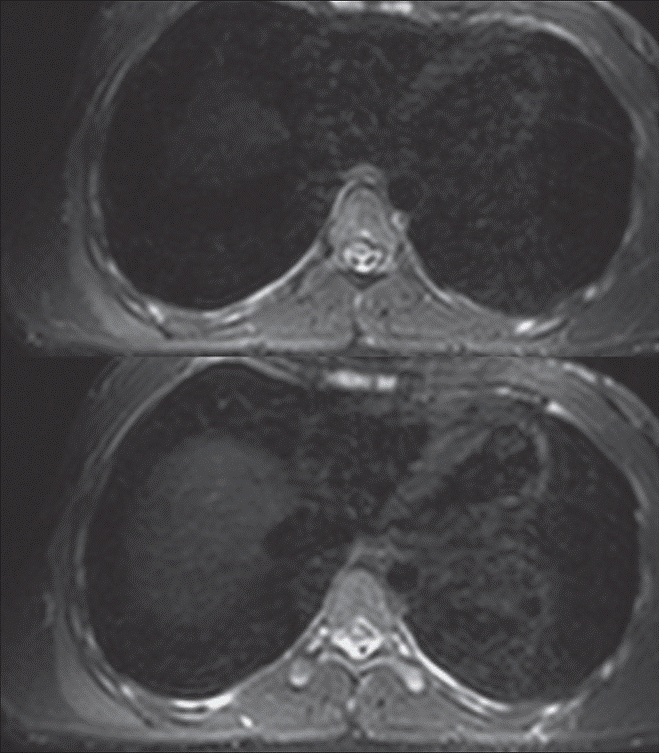
Fig. 2: Axial consecutive STIR MR images.
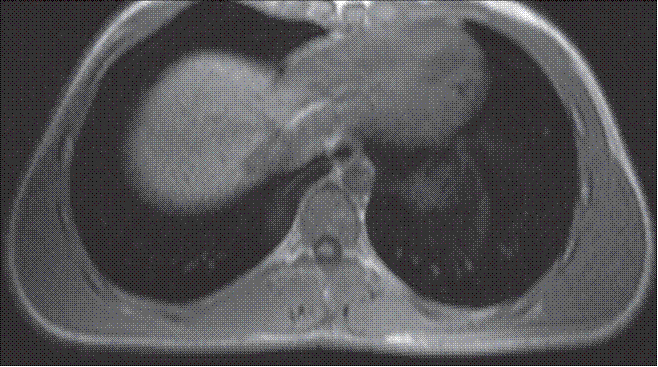
Fig. 3: Axial T1W MR image.
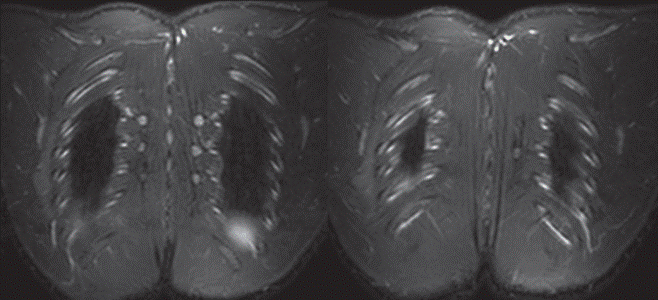
Fig. 4: Coronal consecutive STIR MR images.
PART B
Diagnosis: Parsonage Turner syndrome
Winging scapula is defined as the wing-like appearance of the medial scapular border and may result from various pathologies related to long thoracic nerve injury and serratus anterior muscle paresis (Fig. 1) [1].
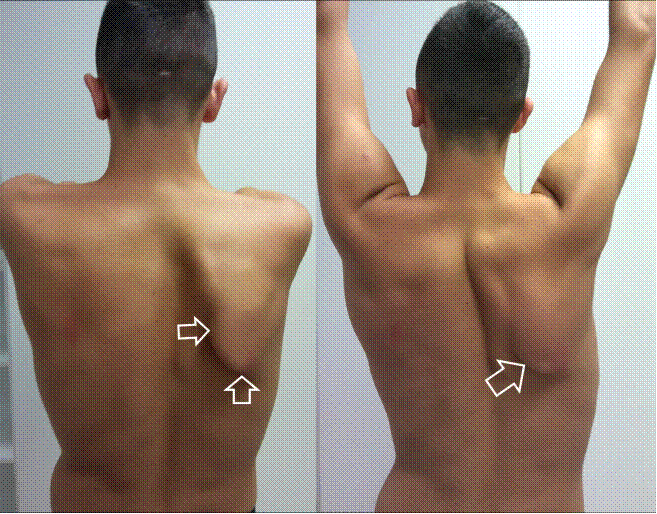
Fig. 1: Winging scapula is the protrusion of the medial border of the scapula from the thorax (arrows).
In our patient there was no history of previous trauma. The EMG showed acute denervation of muscles, a finding which is consistent with Parsonage Turner syndrome (PTs). The muscles involved were the anterior serratus and trapezius, innervated by the long thoracic and spinal accessory nerves respectively. MR images showed accordingly the muscular oedema (Figs. 2-4).
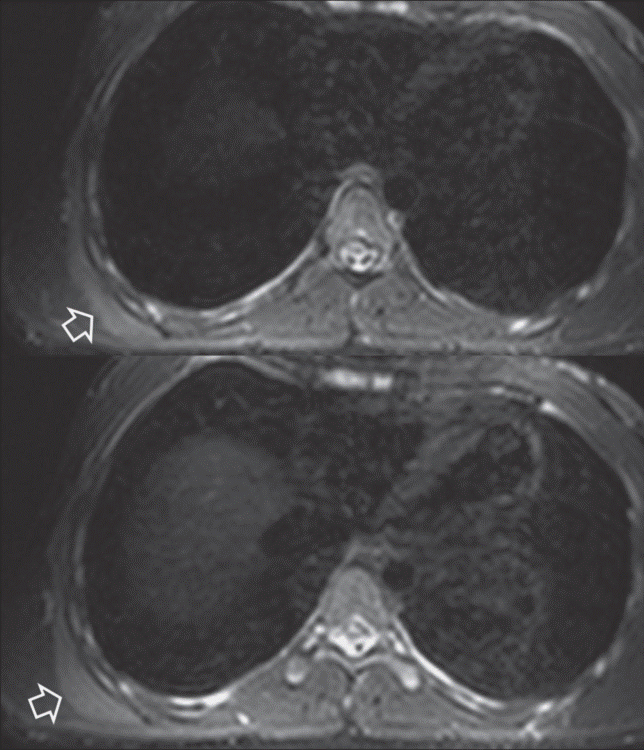
Fig. 2: Axial consecutive STIR MR images show oedema and mild swelling of the right serratus anterior muscle (arrows).
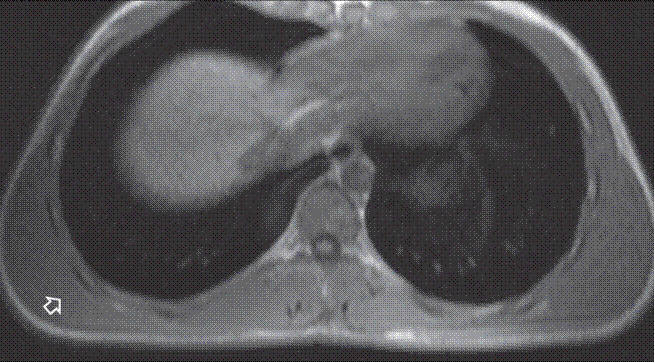
Fig. 3: Axial T1W MR image does not show any atrophy or fatty infiltration of the anterior serratus muscle (arrow).
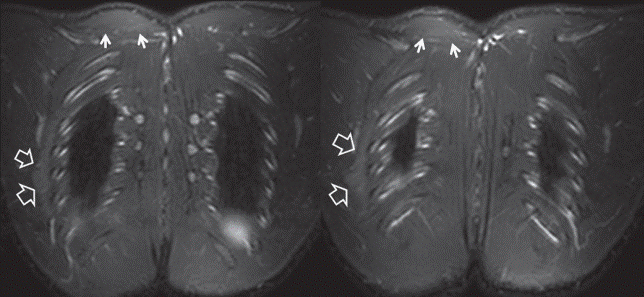
Fig. 4: Coronal consecutive STIR MR images show oedema and mild swelling of the right serratus anterior muscle (open arrows) and of the right trapezius muscle (arrows).
PTs, also known as neuralgic amyotrophy or branchial plexus neuritis, is a rare, self limited disorder of the branchial plexus [2], which usually affects the long thoracic, axillary, radial or phrenic nerves [3]. PTs diagnosis requires previous exclusion of a brachial plexus lesion. It is characterised by the inflammation of the nerves that innervate the muscles of the chest, shoulders and arms [2]. Its cause is not well defined but viral and immunological patterns are suggested [3]. This syndrome may appear in two different forms, idiopathic or hereditary [4]. The aetiology of the idiopathic pattern remains unclear [2] and an immune cause has been suggested [4]. Multiple antecedent events such as viral infection, trauma, strenuous exercise and surgery may trigger an immune-mediated syndrome [4, 5]. As far as the hereditary pattern is concerned, it is an autosomal-dominant recurrent neuropathy of the branchial plexus due to defects in a septin family gene. Mutations in the gene septin 9 on chromosome 17q23 are detected in families with hereditary form of the syndrome [4]. The overall incidence is about 1.64 per 100,000, usually affecting people between 30 and 70 years and mainly men [5], with ratios ranging from 2:1 to 11.5:1 [6]. It was believed that the long thoracic nerve was the nerve mainly affected in PTs, but later reports have shown a higher incidence of isolated suprascapular nerve involvement. Furthermore, the axillary, radial and phrenic nerves or even the entire branchial plexus may be affected [3]. This syndrome appears bilaterally in up to one third of the patients [5].
Clinically, PTs presents with acute, severe neurogenic pain in the shoulder or arm lasting for days or weeks. Pain is often unrelenting; it worsens with shoulder movements and can also worsen at night, awaking patients from sleep [4, 7]. It is often described as constant, sharp, stabbing, throbbing, or aching pain. Characteristically it is located in the shoulder and often radiates into the arm or neck, commonly aggravated by movement of the shoulder but not typically by movement of the neck or Valsalva maneuvers [7]. Pain is usually followed by muscle weakness, atrophy, paraesthesia and hypoaesthesia. Muscle weakness typically begins to develop days to weeks after the onset of pain and often worsens as the pain subsides [4, 7]. The initial pain location does not necessarily correlate to the muscle weakness distribution and does not always correlate with a single nerve root distribution. Multiple muscles may be involved which do not coincide with a single or specific nerve affliction. Upper brachial plexus involvement is the most common pattern [4]. Atrophy of the involved muscles usually occurs relatively quickly [7]. Hypoaesthesia and paraesthesia are the most commonly described sensory symptoms and the sensory loss is often patchy in distribution, corresponding to the sites of plexus or nerve involvement [4]. Autonomic symptoms have rarely been described, including trophic skin changes, oedema in the involved extremity, temperature dysregulation, changes in nail or hair growth and increased sweating [4, 7].
The diagnosis of PTs is mainly clinical but no specific tests exist. Therefore, as PTs could be confused with other diseases, such as neoplastic plexopathy, imaging is required for accurate diagnosis, which will guide proper treatment. There is no surgical treatment for PTs. Analgesics and/or non-steroidal anti-inflammatory drugs along with physiotherapy usually result in full recovery within three years with a low percentage of relapse. Imaging is important in order to exclude common disorders, such as denervation from ganglion cysts or other mass-like lesions [4]. MR imaging is the method of choice, by revealing, on fluid-sensitive sequences, diffusely increased signal in various muscles in the early stages. In chronic disease, atrophy, demonstratedwith reduction in muscle bulk and increased T1 signal due to fatty infiltration are shown. Intramuscular signal may return to normal several months after symptom onset but cases with atrophy and fatty infiltration correspond to irreversible changes [4]. EMG testing is also useful, revealing acute denervation in various muscles [3]. In our patient, full recovery was observed on the three-months clinical follow up and thus there was no need for further imaging. R
Conflict of interest
The authors declared no conflicts of interest.
Key words
Parsonage Turner syndrome; MR imaging/diagnosis
References
1. Gooding BW, Geoghegan JM, Wallace WA, et al. Scapular winging. Shoulder Elbow 2014; 6(1): 4-11.
2. Zara G, Gasparotti R, Manara R. MR imaging of peripheral nervous system involvement: Parsonage-Turner Syndrome. J Neurol Sci 2012; 315(1-2): 170-171.
3. Bencardino JT, Rosenberg ZS. Entrapment neuropathies of the shoulder and elbow in the athlete. Clin Sports Med 2006; 25(3): 465-487.
4. Stutz CM. Neuralgic amyotrophy: Parsonage-Turner syndrome. J Hand Surg Am 2010; 35(12): 2104-2106.
5. Yanny S, Toms AP. MR patterns of denervation around the shoulder. AJR Am J Roentgenol 2010; 195(2): W157-163.
6. Scalf RE, Wenger DE, Frick MA, et al. MRI findings of 26 patients with Parsonage-Turner syndrome. AJR Am J Roentgenol 2007; 189(1): W39-44.
7. Smith CC, Bevelaqua AC. Challenging pain syndromes: Parsonage-Turner syndrome. Phys Med Rehabil Clin N Am 2014; 25(2): 265-277.
Ready - Made Citation
Terezaki F, Savva ED, Smarlamaki RM. Winging scapula in a young athletic male. Hell J Radiol 2018; 3(2): 80-85.